BLOG AND RESOURCES
Check back often for blog posts and resources from our team!


Medical Interpreting: Why Professional Language Services Matter in Healthcare
A topic that surfaces frequently in spaces like OCR complaint investigations and malpractice depositions more often than most administrators realize: the use of unqualified interpreters in clinical settings.
From the emergency department to the surgical suite, language barriers affect patient safety every single day. The good news? The solutions are clear, the standards are established, and the business case for investing in professional interpretation has never been stronger.
Read on for our in-depth feature, compliance reminders, and a quick self-assessment for your organization.
At a Glance
25+ million Americans have Limited English Proficiency (LEP)
LEP patients experience adverse events at twice the rate of English-proficient patients when no interpreter is present
Why "Good Enough" Isn't Good Enough
When a patient speaks limited English, the temptation to rely on whoever is available (a bilingual colleague, a family member, even a smartphone translation app) is understandable. It feels like a practical solution in a resource-constrained environment.
It isn't.
Untrained interpreters introduce errors. Family members filter information, consciously or not. Children who interpret for parents are exposed to information they are not equipped to process. Staff interpreters pulled from other duties lack the specialized medical vocabulary that clinical interpretation demands.
The consequences range from incorrect diagnoses and medication errors to compromised informed consent and catastrophic adverse outcomes. The legal exposure (from HIPAA violations to Title VI complaints to malpractice litigation) is substantial.
Professional, certified medical interpreters change this equation entirely.
What Certified Interpreters Bring to the Encounter
A Certified Medical Interpreter (CMI) or Certified Healthcare Interpreter (CHI) has demonstrated:
Fluency and proficiency in both languages, assessed by standardized examination
Mastery of specialized medical terminology across clinical specialties
Training in the ethical principles of accuracy, impartiality, and confidentiality
Knowledge of cultural health beliefs that affect patient communication
Protocols for managing difficult conversations: psychiatric emergencies, end-of-life discussions, trauma disclosures
This helps providers get complete, accurate information. Patients truly understand their diagnosis, treatment, and options. Informed consent is meaningful, not performative.
Compliance Snapshot: What the Law Requires
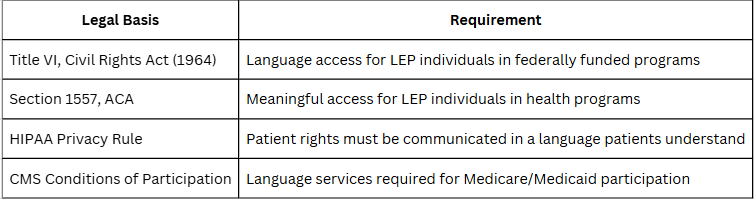
Note: Using a family member or untrained staff does not satisfy these requirements.
CLINICAL FOCUS: HIGH-RISK SCENARIOS
The demand for medical interpreters is not uniform across your facility. These settings carry the highest risk when language access fails:
🔴 Emergency Department: Triage errors and missed symptom reports are a documented risk. Patients cannot effectively describe onset, character, or severity of symptoms without a trained interpreter.
🔴 Surgical Informed Consent: Consent obtained without verified patient comprehension is legally vulnerable. Surgeons and OR teams must have confidence that patients understand what they are agreeing to.
🔴 Psychiatric Evaluations: Mental status examination, risk assessment, and therapeutic rapport all depend on nuanced language. Automated tools and ad-hoc interpretation are especially inappropriate here.
🔴 Medication Discharge Instructions: Post-discharge medication errors are a primary driver of 30-day readmissions. Complex dosing schedules, side effect warnings, and drug interaction information must be understood, not merely delivered.
QUICK ORGANIZATIONAL SELF-ASSESSMENT
Take 5 minutes with your team this week. Can you answer "yes" to each of the following?
☐ We have a written language access plan that is reviewed annually.
☐ Our interpreters are certified (CMI, CHI, or equivalent state credential).
☐ Staff know how to request an interpreter and when it is required.
☐ We never use patients' minor children as interpreters.
☐ Our interpreter services vendor has a signed HIPAA Business Associate Agreement.
☐ We track interpreter utilization data and use it for quality improvement.
☐ Clinical staff have received training on working effectively with medical interpreters.
If you answered "no" to two or more items, your organization has a meaningful language access gap. This month is a good time to close it.
CERTIFICATION CORNER
Q: Which certification should we require for medical interpreters?
The two nationally recognized healthcare interpreter certifications are:
CMI (Certified Medical Interpreter): Issued by the National Board of Certification for Medical Interpreters (NBCMI). Requires written and oral examination, 40 hours of verified training, and language proficiency assessment.
CHI (Certified Healthcare Interpreter): Issued by the Certification Commission for Healthcare Interpreters (CCHI). Also requires written and oral examination and continuing education for recertification.
Both are rigorous, nationally recognized, and accepted by accrediting bodies including The Joint Commission.
For languages where national certification does not yet exist: consider requiring a minimum of 40 hours of accredited interpreter training, documented language proficiency, and demonstrated adherence to the National Code of Ethics for Healthcare Interpreters.
BY THE NUMBERS
$71 million: malpractice judgment in a landmark case where a family member's mistranslation of "intoxicado" (nauseated/poisoned) as "intoxicated" led to misdiagnosis and permanent paralysis.
2x: the rate of serious adverse events for LEP patients when professional interpreters are not used, compared to English-proficient patients. (Source: Health Affairs)
40 hours: minimum interpreter training required to sit for national certification exams.
$280: estimated average cost of professional on-site interpretation for a complex medical encounter. Compare to the average cost of a single adverse event.
RESOURCE OF THE MONTH
National Standards for Healthcare Interpreters (NCIHC) The National Council on Interpreting in Health Care has published the definitive standards of practice and code of ethics for medical interpreters in the United States. Available at: ncihc.org
CONNECT WITH US
Have a language access challenge you'd like us to address? A success story to share? Reply to this newsletter. We read every response.
📧 [email protected] 📞 240-233-6080 🌐 www.stratalang.com
© 2026 Strata Language Services. All rights reserved.
Disclaimer: The information provided in this article is intended for general informational and educational purposes only and does not constitute legal, medical, or compliance advice. While every effort has been made to ensure the accuracy of the content at the time of publication, laws, regulations, and industry standards governing language access and healthcare interpretation are subject to change. Healthcare organizations should consult qualified legal counsel and compliance professionals to evaluate their specific obligations under applicable federal, state, and local laws, including but not limited to Title VI of the Civil Rights Act, Section 1557 of the Affordable Care Act, HIPAA, and CMS Conditions of Participation. The statistics and research findings cited are drawn from publicly available sources and are provided for illustrative purposes. Individual outcomes and organizational requirements will vary.

• Veteran-Owned Small Business
(CVE certified)
• Woman-Owned Small Business
• Maryland-Certified MBE/DBE/SBE

A multilayered approach to translating

©2026 By Strata Language Services | Privacy Policy
